After successfully treating skin cancer, many patients find themselves facing a new challenge: the reconstruction and restoration of the treated area. While the primary focus during treatment is eliminating cancerous cells, the resulting wound or surgical site often requires careful consideration to achieve optimal healing and cosmetic outcomes.
Keep reading to learn more about skin cancer reconstruction, including what happens during the procedure and what different options are available.
What Is Skin Cancer Reconstruction?
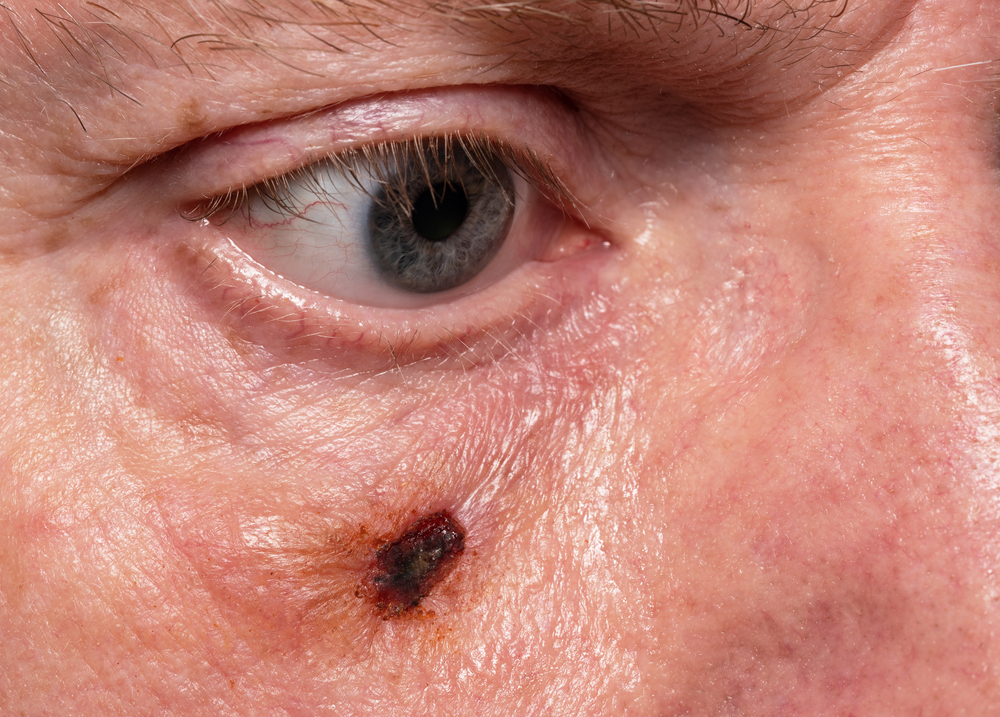
Skin cancer reconstruction refers to the surgical techniques used to repair and restore skin after cancer removal. The goal is to close the surgical wound while maintaining proper function and achieving the best possible cosmetic result for the treated area.
The type and extent of reconstruction needed depend on several factors, including the size and location of the cancer, the depth of tissue removal, and the patient’s individual healing characteristics. Some cases may require simple closure techniques, while others might need more complex reconstruction procedures.
Types of Skin Cancer Reconstruction
Primary Closure
Primary closure is the simplest form of reconstruction, where the edges of the wound are brought together and closed linearly with sutures. This technique works best for smaller lesions where there’s sufficient laxity of the surrounding skin to close the wound without tension. This method is often preferred when the cancer site allows for this approach without compromising the final appearance.
Skin Grafts
When primary closure isn’t possible due to the size of the defect, skin grafts may be necessary. This technique involves taking healthy skin from another part of the body (donor site) and transplanting it to cover the open wound.
There are two main types of skin grafts: split-thickness grafts, which include only the top layers of skin, and full-thickness grafts, which include all layers of skin. The choice between these options depends on the specific characteristics of the wound and the desired cosmetic outcome.
Dr. Grace Sohn, a fellowship-trained and board-certified Mohs surgeon at Golden State Dermatology, explains the importance of proper graft selection:
“Choosing the right type of skin graft and donor site is crucial for both proper healing and optimal cosmetic results. We carefully consider the location of the defect, the patient’s skin characteristics, and lifestyle when determining the best grafting approach. While the process may seem complex, skin grafts are an important tool in your surgeon’s arsenal to restore both function and appearance to the treated area.”
Local Flaps
Local flaps involve moving nearby healthy tissue to cover the wound while maintaining its blood supply. This technique often provides better color and texture matching compared to skin grafts since the tissue comes from the same general area.
Various flap designs can be used depending on the wound characteristics and surrounding tissue availability. The advantage of local flaps is that they typically heal well and provide excellent cosmetic results with proper technique.
Regional and Distant Flaps
For larger or more complex defects, regional or distant flaps may be necessary. While these techniques are more complex, they can provide excellent outcomes for challenging reconstruction cases.
Factors Influencing Reconstruction Choice
Several important considerations guide the selection of the most appropriate reconstruction technique for each patient. Your dermatologic surgeon will carefully evaluate these factors to develop a personalized treatment plan.
Location of the Cancer
The location of the skin cancer significantly impacts reconstruction options. Facial areas, particularly around the eyes, nose, and mouth, require special consideration due to the importance of maintaining proper function and appearance.
Areas with high mobility, such as joints, may require specific reconstruction techniques to preserve movement and flexibility. Your dermatologic surgeon will consider how the reconstruction will affect the function of the treated area.
Cosmetically sensitive areas often benefit from more sophisticated reconstruction techniques, even if they require additional surgical stages. The goal is always to achieve the best possible outcome while ensuring complete cancer removal.
Size and Depth of the Defect
Larger wounds typically require more complex reconstruction techniques. The depth of tissue removal also influences the choice of reconstruction method, as deeper defects may need more substantial repair.
The three-dimensional characteristics of the wound help determine whether simple closure, grafting, or flap reconstruction will provide the best outcome. Your surgeon will assess these factors during the treatment planning process.
Patient’s Overall Health
Your general health status and healing ability play important roles in reconstruction planning. Age, lifestyle factors, and personal preferences are also considered when developing your reconstruction plan.
The Reconstruction Timeline
Immediate Reconstruction
In many cases, reconstruction is performed immediately following cancer removal during the same surgical session. Immediate reconstruction also reduces the psychological impact of having an open wound and allows for faster return to normal activities.
Katie Given, MD, PhD, a board-certified dermatologist and Mohs Surgeon at Golden State Dermatology, shares her perspective on timing decisions:
“One of the key advantages of Mohs surgery is the ability to completely remove the cancer and perform the necessary reconstruction in a single visit. The procedure is done under local anesthesia in an outpatient setting, allowing for efficient and effective care. When the wound can be closed on the same day as cancer removal, it can help reduce patient discomfort, may lower the risk of infection, and promotes faster recovery.”
Delayed Reconstruction
Sometimes, reconstruction may be delayed to allow for proper healing or to ensure all cancer has been completely removed. Delayed reconstruction gives the surgical site time to heal and allows for thorough margin assessment.
Staged Reconstruction
Complex cases may require staged reconstruction, where the repair is completed in multiple surgical sessions. Your surgeon will explain the timeline and expectations for each stage if this approach is recommended.
What to Expect During Recovery
The recovery process varies depending on the type of reconstruction performed, but most patients can expect some initial swelling and discomfort. Following your surgeon’s post-operative instructions carefully is crucial for optimal healing and the best cosmetic outcome.
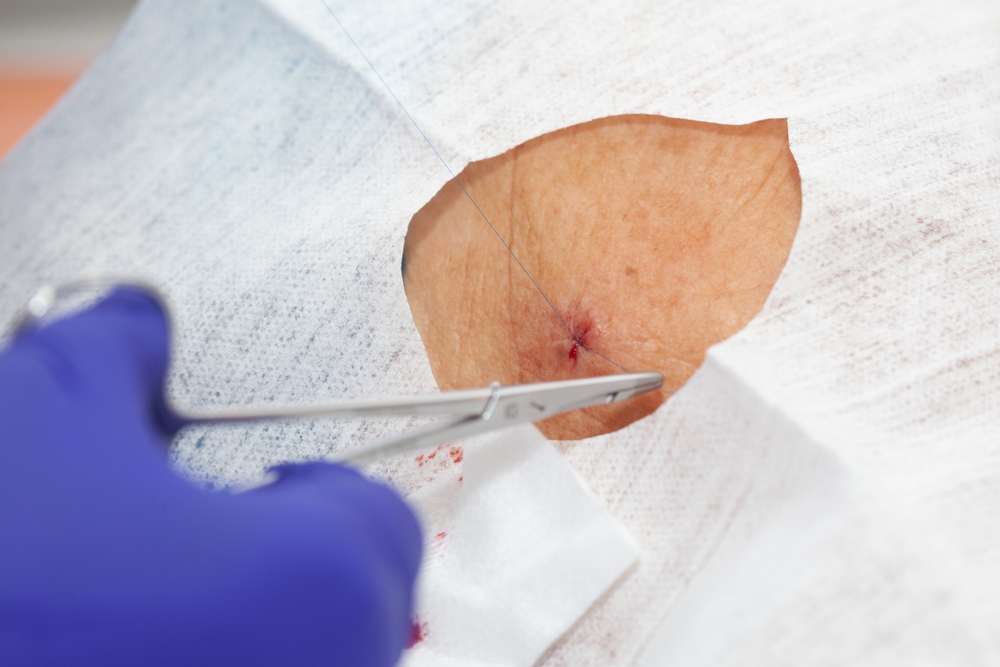
Recovery timelines can range from a few weeks for simple closures to several months for more complex reconstructions. Your dermatologic surgeon will provide specific expectations based on your procedure and individual healing characteristics.
Pain management is typically straightforward, with most patients using over-the-counter medications for any discomfort. Prescription pain medication may be provided for more extensive procedures, though most patients find they need it for only a few days.
Activity restrictions vary based on the location and type of reconstruction performed. Your surgeon will provide detailed guidelines about when you can resume normal activities, exercise, and work responsibilities.
Follow-up appointments are essential for monitoring healing and addressing any concerns that may arise. These visits allow your surgeon to assess the reconstruction progress and make any necessary adjustments to your care plan.
Schedule Your Consultation
Understanding your options for skin cancer reconstruction empowers you to make informed decisions about your treatment and recovery. The experienced team at Duncan Dermatology is committed to providing comprehensive care that addresses both medical and cosmetic concerns.
If you have questions about your skin, schedule an appointment at Duncan Dermatology today!